|
Biaxial chairs enable exact positional testing and treatment. These issues have obviously been a contributing factor to the development of the three biaxial chairs for the reposition of BPPV: the Epley Omniax Rotator, the TRV reposition chair, and the rather new Rotundum positioning chair. In addition, the recurrence rates of BPPV have been reported to be as high as 27% within the first 6 months and 40–50% after 5 years of follow-up. When considering the incidence of the disease, the proportion of patients with unresolved BPPV who might benefit from better treatments is, therefore, potentially quite large. Lateral-canal BPPV, multicanal BPPV, and cupulolithiasis-type BPPV are found to be more difficult to treat thus, 10–20% of all BPPV cases may be challenging to both diagnose and treat. This procedure has a reported efficacy rate of 80% when treating posterior canalolithiasis BPPV. One of the most validated CRPs is the Epley maneuver developed by John Epley in 1992. Several canalith repositioning procedures (CRPs) exist. Despite both conservative and active treatment, several patients still experience persistent BPPV. īenign Paroxysmal Positional Vertigo often resolves within days or weeks without treatment, but early treatment can shorten the duration of the disease and improve quality of life. The Dix-Hallpike maneuver (DH) and the supine roll test (SRT) are two common positional tests and, when used in combination, they test all six SCCs of BPPV. Ī diagnosis of BPPV requires both subjective symptoms (by means of positional vertigo) and objective observation of nystagmus triggered during specific positional tests. Lateral-canal BPPV occurs in 5–15% of all BPPV cases, whereas anterior-canal BPPV and multicanal BPPV occurs only in a few percentage of BPPV cases. By far, posterior-canal BPPV is the most common subtype, including 85–95% of all BPPV cases, most likely because of its anatomical relation to the utricle. Therefore, BPPV may be categorized as anterior-canal BPPV, lateral-canal BPPV, and/or posterior-canal BPPV occurring either uni- or bilaterally or as multicanal BPPV and further classified as being either canalolithiasis or cupulolithiasis. Furthermore, BPPV can be subcategorized according to the affected SCC(s). 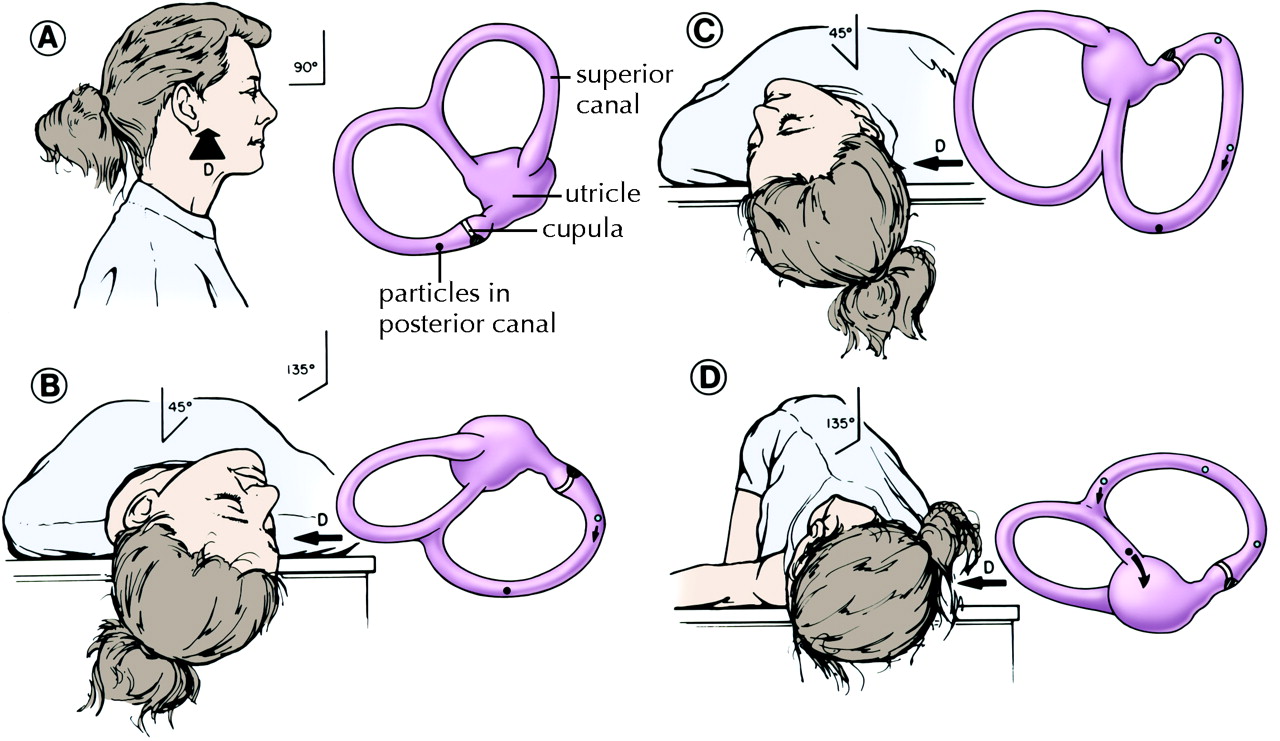
Free-floating otoconia are named canalolithiasis, and otoconia attached to the cupula are named cupulolithiasis. Ĭategorization of BPPV is based on whether the otoconia are floating freely within the endolymph of the SCCs or if otoconia are attached to the cupula. Disequilibrium in signals from the vestibular system results in a rotatory sensation (i.e., vertigo). 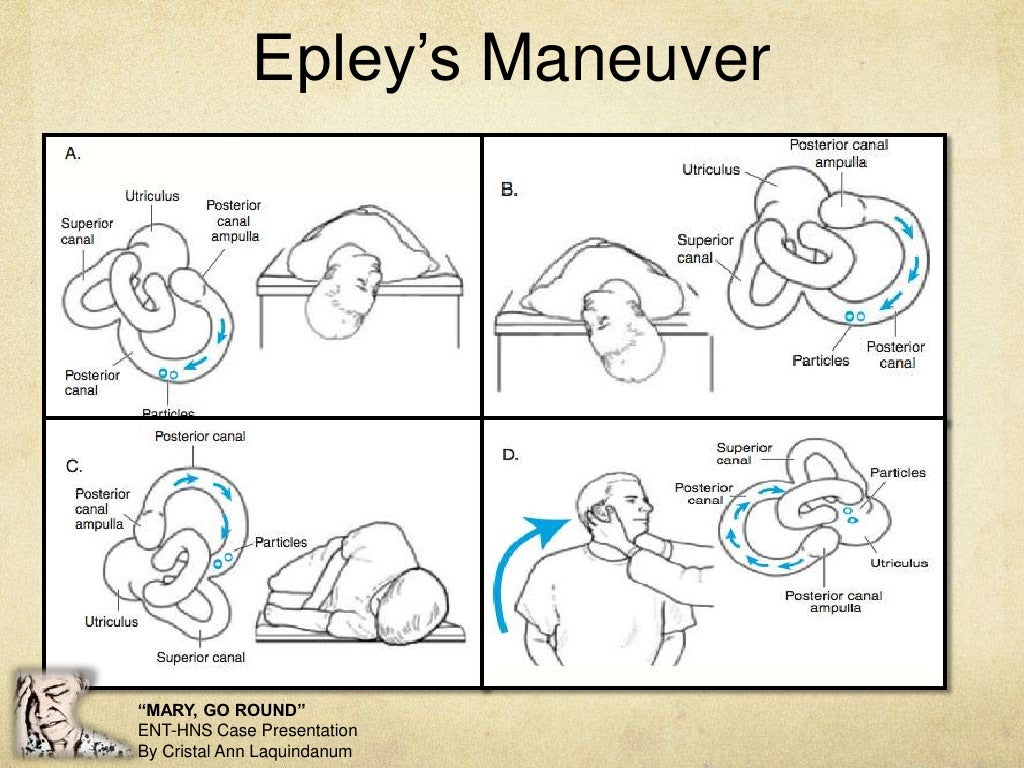
These dislocated otoconia affect the sensory hair cells during movement via their mass, thereby creating an imbalance of signals sent to the central nervous system. Pathophysiologically, BPPV consists of otoconia from the utricle, which are dislocated into one or several of the semicircular canals (SCCs). Usually symptoms are short-lasting (seconds) and emerge when the patient turns their head, looks up, or turns over in bed. īenign Paroxysmal Positional Vertigo is characterized by positional vertigo, which is defined as a rotating sensation induced by position changes relative to gravity. One study estimated that 9% of elderly patients undergoing geriatric assessment for nonbalance-related complaints, suffer from BPPV. 
The incidence rises with increasing age, and the disease is typically seen in patients between 50 and 70 years of age, predominantly women. 
Benign paroxysmal positional vertigo (BPPV) is the most common cause of vertigo, with an incidence between 10.7 and 64.0 cases per 100,000 persons, equivalent to a lifetime prevalence of 2.4%.
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
